Abstract
In some patients, COVID-19 can trigger neurological symptoms with unclear pathogenesis. Here we describe a microphysiological system integrating alveolus and blood–brain barrier (BBB) tissue chips that recapitulates neuropathogenesis associated with infection by SARS-CoV-2. Direct exposure of the BBB chip to SARS-CoV-2 caused mild changes to the BBB, and infusion of medium from the infected alveolus chip led to more severe injuries on the BBB chip, including endothelial dysfunction, pericyte detachment and neuroinflammation. Transcriptomic analyses indicated downregulated expression of the actin cytoskeleton in brain endothelium and upregulated expression of inflammatory genes in glial cells. We also observed early cerebral microvascular damage following lung infection with a low viral load in the brains of transgenic mice expressing human angiotensin-converting enzyme 2. Our findings suggest that systemic inflammation is probably contributing to neuropathogenesis following SARS-CoV-2 infection, and that direct viral neural invasion might not be a prerequisite for this neuropathogenesis. Lung–brain microphysiological systems should aid the further understanding of the systemic effects and neurological complications of viral infection.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$99.00 per year
only $8.25 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Data availability
The main data supporting the results in this study are available within the paper and its Supplementary Information. The raw RNA-seq data are available from the Sequence Read Archive via the accession number PRJNA764053. All data generated or analysed during the study are available from the corresponding authors on reasonable request. Source data are provided with this paper.
Change history
31 October 2023
A Correction to this paper has been published: https://doi.org/10.1038/s41551-023-01141-y
References
Burks, S. M., Rosas-Hernandez, H., Alejandro Ramirez-Lee, M., Cuevas, E. & Talpos, J. C. Can SARS-CoV-2 infect the central nervous system via the olfactory bulb or the blood–brain barrier? Brain Behav. Immun. 95, 7–14 (2021).
Mao, L. et al. Neurologic manifestations of hospitalized patients with coronavirus disease 2019 in Wuhan, China. JAMA Neurol. 77, 683–690 (2020).
Varatharaj, A. et al. Neurological and neuropsychiatric complications of COVID-19 in 153 patients: a UK-wide surveillance study. Lancet Psychiatry 7, 875–882 (2020).
Moriguchi, T. et al. A first case of meningitis/encephalitis associated with SARS-coronavirus-2. Int. J. Infect. Dis. 94, 55–58 (2020).
Bhalerao, A. et al. In vitro modeling of the neurovascular unit: advances in the field. Fluids Barriers CNS 17, 22 (2020).
Oddo, A. et al. Advances in microfluidic blood–brain barrier (BBB) models. Trends Biotechnol. 37, 1295–1314 (2019).
Michael, B. D. et al. Astrocyte- and neuron-derived CXCL1 drives neutrophil transmigration and blood–brain barrier permeability in viral encephalitis. Cell Rep. 32, 108150 (2020).
He, Q. et al. Herpes simplex virus 1-induced blood–brain barrier damage involves apoptosis associated with GM130-mediated Golgi stress. Front Mol. Neurosci. 13, 2 (2020).
Cle, M. et al. Zika virus infection promotes local inflammation, cell adhesion molecule upregulation, and leukocyte recruitment at the blood–brain barrier. mBio 11, e01183-20 (2020).
Thakur, K.T. et al. COVID-19 neuropathology at Columbia University Irving Medical Center/New York Presbyterian Hospital. Brain 144, 2696–2708 (2021).
Matschke, J. et al. Neuropathology of patients with COVID-19 in Germany: a post-mortem case series. Lancet Neurol. 19, 919–929 (2020).
Reichard, R. R. et al. Neuropathology of COVID-19: a spectrum of vascular and acute disseminated encephalomyelitis (ADEM)-like pathology. Acta Neuropathol. 140, 1–6 (2020).
Douaud, G. et al. SARS-CoV-2 is associated with changes in brain structure in UK Biobank. Nature 604, 697–707 (2022).
Krasemann, S. et al. The blood–brain barrier is dysregulated in COVID-19 and serves as a CNS entry route for SARS-CoV-2. Stem Cell Rep. 17, 307–320 (2022).
Jiao, L. et al. The olfactory route is a potential way for SARS-CoV-2 to invade the central nervous system of rhesus monkeys. Signal Transduct. Target Ther. 6, 169 (2021).
Song, E. et al. Neuroinvasion of SARS-CoV-2 in human and mouse brain. J. Exp. Med. 218, e20202135 (2021).
Zhang, L. et al. SARS-CoV-2 crosses the blood–brain barrier accompanied with basement membrane disruption without tight junctions alteration. Signal Transduct. Target Ther. 6, 337 (2021).
Yinda, C. K. et al. K18-hACE2 mice develop respiratory disease resembling severe COVID-19. PLoS Pathog. 17, e1009195 (2021).
Jiang, R. D. et al. Pathogenesis of SARS-CoV-2 in transgenic mice expressing human angiotensin-converting enzyme 2. Cell 182, 50–58.e58 (2020).
Zhang, B. Z. et al. SARS-CoV-2 infects human neural progenitor cells and brain organoids. Cell Res. 30, 928–931 (2020).
Ramani, A. et al. SARS-CoV-2 targets neurons of 3D human brain organoids. EMBO J. 39, e106230 (2020).
Bullen, C. K. et al. Infectability of human BrainSphere neurons suggests neurotropism of SARS-CoV-2. ALTEX 37, 665–671 (2020).
McMahon, C. L., Staples, H., Gazi, M., Carrion, R. & Hsieh, J. SARS-CoV-2 targets glial cells in human cortical organoids. Stem Cell Rep. 16, 1156–1164 (2021).
Pellegrini, L. et al. SARS-CoV-2 infects the brain choroid plexus and disrupts the blood–CSF barrier in human brain organoids. Cell Stem Cell 27, 951–961.e955 (2020).
Jacob, F. et al. Human pluripotent stem cell-derived neural cells and brain organoids reveal SARS-CoV-2 neurotropism predominates in choroid plexus epithelium. Cell Stem Cell 27, 937–950.e939 (2020).
Bhatia, S. N. & Ingber, D. E. Microfluidic organs-on-chips. Nat. Biotechnol. 32, 760–772 (2014).
Abaci, H. E. & Shuler, M. L. Human-on-a-chip design strategies and principles for physiologically based pharmacokinetics/pharmacodynamics modeling. Integr. Biol. 7, 383–391 (2015).
Huh, D. et al. Reconstituting organ-level lung functions on a chip. Science 328, 1662–1668 (2010).
Vatine, G. D. et al. Human iPSC-derived blood–brain barrier chips enable disease modeling and personalized medicine applications. Cell Stem Cell 24, 995–1005.e1006 (2019).
Ahn, S. I. et al. Microengineered human blood–brain barrier platform for understanding nanoparticle transport mechanisms. Nat. Commun. 11, 175 (2020).
Bhise, N. S. et al. A liver-on-a-chip platform with bioprinted hepatic spheroids. Biofabrication 8, 014101 (2016).
Knowlton, S. & Tasoglu, S. A bioprinted liver-on-a-chip for drug screening applications. Trends Biotechnol. 34, 681–682 (2016).
Agarwal, A., Goss, J. A., Cho, A., McCain, M. L. & Parker, K. K. Microfluidic heart on a chip for higher throughput pharmacological studies. Lab Chip 13, 3599–3608 (2013).
Ugolini, G. S., Visone, R., Cruz-Moreira, D., Mainardi, A. & Rasponi, M. Generation of functional cardiac microtissues in a beating heart-on-a-chip. Methods Cell. Biol. 146, 69–84 (2018).
Brown, J. A. et al. Metabolic consequences of inflammatory disruption of the blood–brain barrier in an organ-on-chip model of the human neurovascular unit. J. Neuroinflammation 13, 306 (2016).
Brown, J. A. et al. Metabolic consequences of interleukin-6 challenge in developing neurons and astroglia. J. Neuroinflammation 11, 183 (2014).
Maoz, B. M. et al. A linked organ-on-chip model of the human neurovascular unit reveals the metabolic coupling of endothelial and neuronal cells. Nat. Biotechnol. 36, 865–874 (2018).
Ronaldson-Bouchard, K. et al. A multi-organ chip with matured tissue niches linked by vascular flow. Nat. Biomed. Eng. 6, 351–371 (2022).
Ortega-Prieto, A. M. et al. 3D microfluidic liver cultures as a physiological preclinical tool for hepatitis B virus infection. Nat. Commun. 9, 682 (2018).
Wang, J. et al. A virus-induced kidney disease model based on organ-on-a-chip: pathogenesis exploration of virus-related renal dysfunctions. Biomaterials 219, 119367 (2019).
Johnson, B. N. et al. 3D printed nervous system on a chip. Lab Chip 16, 1393–1400 (2016).
Junaid, A. et al. Ebola hemorrhagic shock syndrome-on-a-chip. iScience 23, 100765 (2020).
Bai, H. et al. Mechanical control of innate immune responses against viral infection revealed in a human lung alveolus chip. Nat. Commun. 13, 1928 (2022).
Si, L. et al. A human-airway-on-a-chip for the rapid identification of candidate antiviral therapeutics and prophylactics. Nat. Biomed. Eng. 5, 815–829 (2021).
Deinhardt-Emmer, S. et al. SARS-CoV-2 causes severe epithelial inflammation and barrier dysfunction. J. Virol. 95, e00110-21 (2021).
Guo, Y. et al. SARS-CoV-2 induced intestinal responses with a biomimetic human gut-on-chip. Sci. Bull. 66, 783–793 (2021).
Thacker, V. V. et al. Rapid endotheliitis and vascular damage characterize SARS-CoV-2 infection in a human lung-on-chip model. EMBO Rep. 22, e52744 (2021).
Zhang, M. et al. Biomimetic human disease model of SARS-CoV-2 induced lung injury and immune responses on organ chip system. Adv. Sci. 8, 2002928 (2020).
Buzhdygan, T. P. et al. The SARS-CoV-2 spike protein alters barrier function in 2D static and 3D microfluidic in-vitro models of the human blood–brain barrier. Neurobiol. Dis. 146, 105131 (2020).
Sungnak, W. et al. SARS-CoV-2 entry factors are highly expressed in nasal epithelial cells together with innate immune genes. Nat. Med. 26, 681–687 (2020).
Zou, X. et al. Single-cell RNA-seq data analysis on the receptor ACE2 expression reveals the potential risk of different human organs vulnerable to 2019-nCoV infection. Front. Med. 14, 185–192 (2020).
Ballabh, P., Braun, A. & Nedergaard, M. The blood–brain barrier: an overview: structure, regulation, and clinical implications. Neurobiol. Dis. 16, 1–13 (2004).
Obermeier, B., Daneman, R. & Ransohoff, R. M. Development, maintenance and disruption of the blood–brain barrier. Nat. Med. 19, 1584–1596 (2013).
Abbott, N. J., Ronnback, L. & Hansson, E. Astrocyte-endothelial interactions at the blood–brain barrier. Nat. Rev. Neurosci. 7, 41–53 (2006).
Bwire, G. M., Majigo, M. V., Njiro, B. J. & Mawazo, A. Detection profile of SARS-CoV-2 using RT-PCR in different types of clinical specimens: a systematic review and meta-analysis. J. Med. Virol. 93, 719–725 (2021).
Wang, W. et al. Detection of SARS-CoV-2 in different types of clinical specimens. JAMA 323, 1843–1844 (2020).
Yu, F. et al. Quantitative detection and viral load analysis of SARS-CoV-2 in infected patients. Clin. Infect. Dis. 71, 793–798 (2020).
Leng, L. et al. Pathological features of COVID-19-associated lung injury: a preliminary proteomics report based on clinical samples. Signal Transduct. Target Ther. 5, 240 (2020).
Walter, L. et al. Nonpsychotropic cannabinoid receptors regulate microglial cell migration. J. Neurosci. 23, 1398–1405 (2003).
Liu, Y. J. et al. Late endosomes promote microglia migration via cytosolic translocation of immature protease cathD. Sci. Adv. 6, eaba5783 (2020).
Lan, X., Han, X., Li, Q., Yang, Q. W. & Wang, J. Modulators of microglial activation and polarization after intracerebral haemorrhage. Nat. Rev. Neurol. 13, 420–433 (2017).
Orihuela, R., McPherson, C. A. & Harry, G. J. Microglial M1/M2 polarization and metabolic states. Br. J. Pharmacol. 173, 649–665 (2016).
Wang, X. & Khalil, R. A. Matrix metalloproteinases, vascular remodeling, and vascular disease. Adv. Pharm. 81, 241–330 (2018).
Raffetto, J. D. & Khalil, R. A. Matrix metalloproteinases and their inhibitors in vascular remodeling and vascular disease. Biochem. Pharmacol. 75, 346–359 (2008).
Bocci, M. et al. Infection of brain pericytes underlying neuropathology of COVID-19 patients. Int. J. Mol. Sci. 22, 11622 (2021).
Cardot-Leccia, N., Hubiche, T., Dellamonica, J., Burel-Vandenbos, F. & Passeron, T. Pericyte alteration sheds light on micro-vasculopathy in COVID-19 infection. Intensive Care Med. 46, 1777–1778 (2020).
Sun, J. et al. Transplantation of hPSC-derived pericyte-like cells promotes functional recovery in ischemic stroke mice. Nat. Commun. 11, 5196 (2020).
Perrin, P. et al. Cytokine release syndrome-associated encephalopathy in patients with COVID-19. Eur. J. Neurol. 28, 248–258 (2021).
Yang, A. C. et al. Dysregulation of brain and choroid plexus cell types in severe COVID-19. Nature 595, 565–571 (2021).
Ghersi-Egea, J. F. et al. Molecular anatomy and functions of the choroidal blood–cerebrospinal fluid barrier in health and disease. Acta Neuropathol. 135, 337–361 (2018).
Lun, M. P., Monuki, E. S. & Lehtinen, M. K. Development and functions of the choroid plexus-cerebrospinal fluid system. Nat. Rev. Neurosci. 16, 445–457 (2015).
Kumari, P. et al. Neuroinvasion and encephalitis following intranasal inoculation of SARS-CoV-2 in K18-hACE2 mice. Viruses 13, 132 (2021).
Iadecola, C., Anrather, J. & Kamel, H. Effects of COVID-19 on the nervous system. Cell 183, 16–27.e11 (2020).
Chen, L. W. et al. Influenza-associated neurological complications during 2014-2017 in Taiwan. Brain Dev. 40, 799–806 (2018).
Radzisauskiene, D., Vitkauskaite, M., Zvinyte, K. & Mameniskiene, R. Neurological complications of pandemic A(H1N1)2009pdm, postpandemic A(H1N1)v, and seasonal influenza A. Brain Behav. 11, e01916 (2021).
Dusedau, H. P. et al. Influenza A virus (H1N1) infection induces microglial activation and temporal dysbalance in glutamatergic synaptic transmission. mBio 12, e0177621 (2021).
Shukla, P., Mandalla, A., Elrick, M. J. & Venkatesan, A. Clinical manifestations and pathogenesis of acute necrotizing encephalopathy: the interface between systemic infection and neurologic injury. Front. Neurol. 12, 628811 (2021).
Barbosa-Silva, M. C. et al. Infectious disease-associated encephalopathies. Crit. Care 25, 236 (2021).
Jeanneret, V., Winkel, D., Risman, A., Shi, H. & Gombolay, G. Post-infectious rhombencephalitis after coronavirus-19 infection: a case report and literature review. J. Neuroimmunol. 357, 577623 (2021).
Hara, M. et al. COVID-19 post-infectious encephalitis presenting with delirium as an initial manifestation. J. Investig. Med. High Impact Case Rep. 9, 23247096211029787 (2021).
Picollet-D’hahan, N., Zuchowska, A., Lemeunier, I. & Le Gac, S. Multiorgan-on-a-chip: a systemic approach to model and decipher inter-organ communication. Trends Biotechnol. 39, 788–810 (2021).
Lyu, Z. et al. A neurovascular-unit-on-a-chip for the evaluation of the restorative potential of stem cell therapies for ischaemic stroke. Nat. Biomed. Eng. 5, 847–863 (2021).
Chen, S. & Schoen, J. Air-liquid interface cell culture: from airway epithelium to the female reproductive tract. Reprod. Domest. Anim. 54, 38–45 (2019).
Jiang, D., Schaefer, N. & Chu, H. W. Air-liquid interface culture of human and mouse airway epithelial cells. Methods Mol. Biol. 1809, 91–109 (2018).
Topol, E. J. COVID-19 can affect the heart. Science 370, 408–409 (2020).
Lee, I. C., Huo, T. I. & Huang, Y. H. Gastrointestinal and liver manifestations in patients with COVID-19. J. Chin. Med Assoc. 83, 521–523 (2020).
Ertuglu, L. A., Kanbay, A., Afsar, B., Elsurer Afsar, R. & Kanbay, M. COVID-19 and acute kidney injury. Tuberk. Toraks 68, 407–418 (2020).
Wang, P., Wu, Y., Chen, W., Zhang, M. & Qin, J. Malignant melanoma-derived exosomes induce endothelial damage and glial activation on a human BBB chip model. Biosensors 12, 89 (2022).
Chomczynski, P. & Sacchi, N. Single-step method of RNA isolation by acid guanidinium thiocyanate-phenol-chloroform extraction. Anal. Biochem. 162, 156–159 (1987).
Rowland, R. & Brandariz-Nunez, A. Analysis of the role of N-linked glycosylation in cell surface expression, function, and binding properties of SARS-CoV-2 receptor ACE2. Microbiol. Spectr. 9, e0119921 (2021).
Acknowledgements
We thank A. P. Xiang (Sun Yat-Sen University) and W. Li (Sun Yat-Sen University) for kindly providing the hPSC-PCs. We thank X. Cheng (Shanghai Institute of Biochemistry and Cell Biology, CAS) for kindly providing the lentivirus–GFP vector. We thank J. Han (Kunming Institute of Zoology, CAS) for helping with blood drawing. This research was supported by the National Key R&D Program of China (number 2022YFA1104700), Strategic Priority Research Program of the CAS (number XDB29050301), National Nature Science Foundation of China (numbers 32101163 and 31971373) and Yunnan Key Research and Development Program (number 202003AD150009).
Author information
Authors and Affiliations
Contributions
J.Q. and P.W. conceived the study. P.W. and L.J. performed the experiments and analysed results. L.J., Z.D., C.W. and Z.L. performed the SARS-CoV-2 infection in the BSL-3 laboratory. M.Z., Y. Wu, W.C., Yaqiong Guo and Y. Wang performed chip fabrication. Yingqi Guo prepared the electron microscopy samples. P.W., J.Q., L.P.L. and R.L. wrote and revised the paper.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Biomedical Engineering thanks Jacquelyn A. Brown, Seung-Woo Cho, John Wikswo and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 SARS-CoV-2 infection caused severe alveolar injury and inflammatory responses on the alveolus chip.
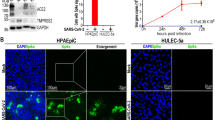
a, Confocal micrographs of alveolar epithelial cells immunostained for E-cadherin (green) and SFTPC (red) on Day 4 following SARS-CoV-2 infection (n = 3). b, Confocal micrographs of pulmonary microvascular endothelial cells immunostained for VE-cadherin (green) on Day 4 following SARS-CoV-2 infection (n = 3). c, Confocal micrographs of alveolar epithelial cells and pulmonary microvascular endothelial cells immunostained for Ki67 (red) on Day 4 following SARS-CoV-2 infection (n = 4). d, Quantification of Ki67+ cells on the mock- and SARS-CoV-2-infected chips based on c. Data are presented as the mean ± SEM and were analyzed using an unpaired Student’s t-test (***: P < 0.001). e, Multiplex cytokine assays showing 13 cytokine concentrations in culture supernatants from the upper epithelial channel (-U) and lower vascular channel (-L) of mock-, or SARS-CoV-2-infected alveolus chips on Day 4 post-infection (n = 3). Data are presented as the mean ± SEM and were analyzed using an unpaired Student’s t-test (***: P < 0.001).
Extended Data Fig. 2 Characterizing immune responses of glial cells and immune cells on the lung–brain MPS.
a, Confocal micrographs of brain endothelial cells immunostained for VE-cadherin and ZO-1 without astrocytes (Δ astrocytes) or without microglia (Δ microglia) following conditioned medium treatment on Day 4 (n = 4). b, Quantification of endothelial cell density based on a. Data are presented as the mean ± SEM and were analyzed using a one-way ANOVA with the Bonferroni post hoc test. c, Confocal micrographs of microglia immunostained for CD206 and F4/80 following conditioned medium treatment on Day 4 (n = 3). d, Quantification of CD206 and F4/80 fluorescence intensity for control and SARS-CoV-2 groups based on c. Data are presented as the mean ± SEM and were analyzed using an unpaired Student’s t-test (***: P < 0.001). e, Fluorescent micrographs of PBMCs (pre-stained with Cell Tracker Red dye) attached to the endothelium following conditioned medium treatment on Day 4 (n = 4). f, Quantification of the density of attached PBMCs based on e. Data are presented as the mean ± SEM and were analyzed using an unpaired Student’s t-test.
Extended Data Fig. 3 SARS-CoV-2 caused injuries of brain pericytes on the lung–brain MPS indirectly.
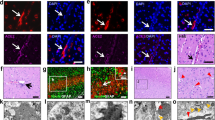
a, Cell morphology and expression of pericyte markers (NG2, CD13 and PDGFRβ) of hPSC-PCs were revealed by bright-field imaging and immunostaining imaging, respectively (n = 3). b, Schematic description of the BBB chip by co-culturing brain endothelial cells, astrocytes, pericytes and microglia. c, A side view of confocal immunofluorescent image showing BBB interface, which was formed by co-culture of human endothelial cells (ZO-1 staining, red), astrocytes (GFAP staining, red) and hPSC-PCs (labeled by GFP, green) under fluid flow conditions for 3 days. The white dotted line indicates the porous membrane. d, Confocal micrographs showing the co-culture of human astrocytes (GFAP staining, red) and hPSC-PCs (labeled by GFP) on the BBB chip (n = 3). e, Confocal micrographs of hPSC-PCs (labeled by GFP) immunostained for viral Spike (red) following conditioned medium treatment (n = 4). f, Quantification of the ratio of hPSC-PCs (green) coverage based on e. Data are presented as the mean ± SEM and were analyzed using an unpaired Student’s t-test. g, Quantification of the hPSC-PCs density based on e. Data are presented as the mean ± SEM and were analyzed using an unpaired Student’s t-test.
Supplementary information
Supplementary Information
Supplementary figures and tables.
Source data
Source Data Fig. 2
Unprocessed western blots.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, P., Jin, L., Zhang, M. et al. Blood–brain barrier injury and neuroinflammation induced by SARS-CoV-2 in a lung–brain microphysiological system. Nat. Biomed. Eng (2023). https://doi.org/10.1038/s41551-023-01054-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41551-023-01054-w
This article is cited by
-
Virus-induced brain pathology and the neuroinflammation-inflammation continuum: the neurochemists view
Journal of Neural Transmission (2024)