Abstract
Objectives
To produce a novel injectable treated dentin matrix hydrogel (TDMH) to be used as a novel pulp-capping agent for dentin regeneration compared with Biodentine and MTA.
Materials and methods
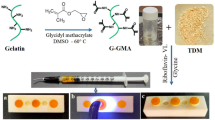
Thirty intact fully erupted premolars scheduled to be extracted for orthodontic reasons were included. Pulps were mechanically exposed in the middle of the cavity floor. TDMH was composed of TDM powder (500-μm particle size) and sodium alginate as an injectable scaffold. The capped teeth were divided into three equal groups (n = 10): TDMH, Biodentine, and MTA respectively. Clinical examination and assessment of periapical response were performed. The teeth were extracted after 2-weeks and 2-month intervals, stained with hematoxylin-eosin, and categorized by using a histologic scoring system. Statistical analysis was performed using chi-square and Kruskal-Wallis test (p = 0.05).
Results
All teeth were vital during observation periods. Histological analysis after 2 months showed complete dentin bridge formation and absence of inflammatory pulp response with no significant differences between groups. However, the formed dentin was significantly thicker with the TDMH group with layers of well-arranged odontoblasts that were found to form a homogenous tubular structure with numerous dentinal tubule lines showing a positive trend to dentin regeneration.
Conclusions
TDMH could achieve dentin regeneration and conservation of pulp vitality and might serve as a feasible natural substitute for silicate-based cements in restoring in vivo dentin defect in direct pulp-capping procedure.
Trial registration
PACTR201901866476410







Similar content being viewed by others
References
Bjørndal L, Mjör IA (2001) Pulp-dentin biology in restorative dentistry Part 4: dental caries – characteristics of lesions and pulpal reactions. Quintessence Int 32:717–736
Paranjpe A, Zhang H, Johnson JD (2010) Effects of mineral trioxide aggregate on human dental pulp cells after pulp-capping procedures. J Endod 36:1042–1047. https://doi.org/10.1016/j.joen.2010.02.013
Gandolfi MG, Siboni F, Botero T, Bossù M, Riccitiello F, Prati C (2015) Calcium silicate and calcium hydroxide materials for pulp capping: biointeractivity, porosity, solubility and bioactivity of current formulations. J Appl Biomater Funct Mater 13:43–60. https://doi.org/10.5301/jabfm.5000201
Collado-González M, García-Bernal D, Oñate-Sánchez RE, Ortolani-Seltenerich PS, Álvarez-Muro T, Lozano A, Forner L, Llena C, Moraleda JM, Rodríguez-Lozano FJ (2017) Cytotoxicity and bioactivity of various pulpotomy materials on stem cells from human exfoliated primary teeth. Int Endod J 50(Suppl2):e19–e30. https://doi.org/10.1111/iej.12751
Moussa DG, Aparicio C (2019) Present and future of tissue engineering scaffolds for dentin-pulp complex regeneration. J Tissue Eng Regen Med 13:58–75. https://doi.org/10.1002/term.2769
Paula AB, Laranjo M, Marto CM, Paulo S, Abrantes AM, Casalta-Lopes J, Marques-Ferreira M, Botelho MF, Carrilho E (2018) Direct pulp capping: what is the most effective therapy?-systematic review and meta-analysis. J Evid Based Dent Pract 18:298–314. https://doi.org/10.1016/j.jebdp.2018.02.002
Horst OV, Chavez MG, Jheon AH, Desai T, Klein OD (2012) Stem cell and biomaterials research in dental tissue engineering and regeneration. Dent Clin N Am 56:495–520. https://doi.org/10.1016/j.cden.2012.05.009
Tran HLB, Nguyen MT, Doan VN (2015) Fabrication and evaluation of human dentin as scaffold for dental pulp stem cells. Tissue Eng Regen Med 12:222–230. https://doi.org/10.1007/s13770-014-0103-y
Li R, Guo W, Yang B, Guo L, Sheng L, Chen G, Li Y, Zou Q, Xie D, An X, Chen Y (2011) Human treated dentin matrix as a natural scaffold for complete human dentin tissue regeneration. Biomaterials 32:4525–4538. https://doi.org/10.1016/j.biomaterials.2011.03.008
Tabatabaei FS, Tatari S, Samadi R, Torshabi M (2016) Surface characterization and biological properties of regular dentin, demineralized dentin, and deproteinized dentin. J Mater Sci Mater Med 27:164. https://doi.org/10.1007/s10856-016-5780-8
Widbiller M, Eidt A, Wölflick M, Lindner SR, Schweikl H, Hiller KA, Buchalla W, Galler KM (2018) Interactive effects of LPS and dentin matrix proteins on human dental pulp stem cells. Int Endod J 51:877–888. https://doi.org/10.1111/iej.12897
Chen J, Cui C, Qiao X, Yang B, Yu M, Guo W, Tian W (2017) Treated dentin matrix paste as a novel pulp capping agent for dentin regeneration. J Tissue Eng Regen Med 11:3428–3436. https://doi.org/10.1002/term.2256
Mehrvarzfar P, Abbott PV, Mashhadiabbas F, Vatanpour M, Savadkouhi S (2018) Clinical and histological responses of human dental pulp to MTA and combined MTA/treated dentin matrix in partial pulpotomy. Aust Endod J 44:46–53. https://doi.org/10.1111/aej.12217
Bidarra SJ, Barrias CC, Granja PL (2014) Injectable alginate hydrogels for cell delivery in tissue engineering. Acta Biomater 10:1646–1662. https://doi.org/10.1016/j.actbio.2013.12.006
Antoine EE, Vlachos PP, Rylander MN (2014) Review of collagen I hydrogels for bioengineered tissue microenvironments: characterization of mechanics, structure, and transport. Tissue Eng B Rev 20:683–696. https://doi.org/10.1089/ten.teb.2014.0086
Tan H, Shen Q, Jia X, Yuan Z, Xiong D (2012) Injectable nanohybrid scaffold for biopharmaceuticals delivery and soft tissue engineering. Macromol Rapid Commun 33:2015–2022. https://doi.org/10.1002/marc.201200360
Cardoso DA, van den Beucken JJ, Both LL, Bender J, Jansen JA, Leeuwenburgh SC (2014) Gelation and biocompatibility of injectable alginate-calcium phosphate gels for bone regeneration. J Biomed Mater Res A 102:808–817. https://doi.org/10.1002/jbm.a.34754
Espona-Noguera A, Ciriza J, Cañibano-Hernández A, Fernandez L, Ochoa I, del Burgo LS, Pedraz JL (2018) Tunable injectable alginate-based hydrogel for cell therapy in Type 1 Diabetes Mellitus. Int J Biol Macromol 107(PtA):1261–1269. https://doi.org/10.1016/j.ijbiomac.2017.09.103
Nowicka A, Lipski M, Parafiniuk M, Sporniak-Tutak K, Lichota D, Kosierkiewicz A, Kaczmarek W, Buczkowska-Radlińska J (2013) Response of human dental pulp capped with biodentine and mineral trioxide aggregate. J Endod 39:743–747. https://doi.org/10.1016/j.joen.2013.01.005
Silva GA, Lanza LD, Lopes-Júnior N, Moreira A, Alves JB (2006) Direct pulp capping with a dentin bonding system in human teeth: a clinical and histological evaluation. Oper Dent 31:297–307. https://doi.org/10.2341/05-65
Bollu IP, Velagula LD, Bolla N, Kumar KK, Hari A, Thumu J (2016) Histological evaluation of mineral trioxide aggregate and enamel matrix derivative combination in direct pulp capping: an in vivo study. J Conserv Dent 19:536–540. https://doi.org/10.4103/0972-0707.194031
Iwamoto CE, Adachi E, Pameijer CH, Barnes D, Romberg EE, Jefferies S (2006) Clinical and histological evaluation of white ProRoot MTA in direct pulp capping. Am J Dent 19:85–90
Medina V, Shinkai K, Shirono M, Tanaka N, Katoh Y (2002) Histopathologic study on pulp response to single-bottle and self-etching adhesive systems. Oper Dent 27:330–342
Asgary S, Ahmadyar M (2013) Vital pulp therapy using calcium-enriched mixture: an evidence-based review. J Conserv Dent 16:92–98. https://doi.org/10.4103/0972-0707.108173
Zarrabi MH, Javidi M, Jafarian AH, Joushan B (2010) Histologic assessment of human pulp response to capping with mineral trioxide aggregate and a novel endodontic cement. J Endod 36:1778–1781. https://doi.org/10.1016/j.joen.2010.08.024
Tran XV, Gorin C, Willig C, Baroukh B, Pellat B, Decup F (2012) Effect of a calcium-silicate-based restorative cement on pulp repair. J Dent Res 91:1166–1171. https://doi.org/10.1177/0022034512460833
Yaemkleebbua K, Osathanon T, Nowwarote N, Limjeerajarus CN, Sukarawan W (2019) Analysis of hard tissue regeneration and Wnt signalling in dental pulp tissues after direct pulp capping with different materials. Int Endod J 52:1605–1616. https://doi.org/10.1111/iej.13162
Grech L, Mallia B, Camilleri J (2013) Investigation of the physical properties of tricalcium silicate cement-based root-end filling materials. Dent Mater 29:e20–e28. https://doi.org/10.1016/j.dental.2012.11.007
De Rossi A, Silva LA, Gatón-Hernández P, Sousa-Neto MD, Nelson-Filho P, Silva RA, de Queiroz AM (2014) Comparison of pulpal responses to pulpotomy and pulp capping with biodentine and mineral trioxide aggregate in dogs. J Endod 40:1362–1369. https://doi.org/10.1016/j.joen.2014.02.006
Camilleri J, Sorrentino F, Damidot D (2013) Investigation of the hydration and bioactivity of radiopacified tricalcium silicate cement, biodentine and MTA angelus. Dent Mater 29:580–593. https://doi.org/10.1016/j.dental.2013.03.007
Giraud T, Jeanneau C, Bergmann M, Laurent P, About I (2018) Tricalcium silicate capping materials modulate pulp healing and inflammatory activity in vitro. J Endod 44:1686–1691. https://doi.org/10.1016/j.joen.2018.06.009
Kim J, Song Y, Min K, Kim S, Koh J, Lee B, Chang HS, Hwang IN, Oh WM, Hwang YC (2016) Evaluation of reparative dentin formation of ProRoot MTA, Biodentine and BioAggregate using micro-CT and immunohistochemistry. Restor Dent Endod 41:29–36. https://doi.org/10.5395/rde.2016.41.1.29
Shayegan A, Jurysta C, Atash R, Petein M, Abbeele A (2012) Biodentine used as a pulp-capping agent in primary pig teeth. Pediatr Dent 34:e202–e28e
Sohn S, Park Y, Srikanth S, Arai A, Song M, Yu B, Shin KH, Kang MK, Wang C, Gwack Y, Park NH (2015) The role of ORAI1 in the odontogenic differentiation of human dental pulp stem cells. J Dent Res 94:1560–1567. https://doi.org/10.1177/0022034515608128
da Silva GS, Moreira MS, Fukushima KA, Raggio DP, Mello-Moura ACV, Lara JS, Gimenez T, Junior SA, Morimoto S, Tedesco TK (2020) Current evidence of tissue engineering for dentine regeneration in animal models: a systematic review. Regen Med 15:1345–1360. https://doi.org/10.2217/rme-2019-0005
Iohara K, Nakashima M, Ito M, Ishikawa M, Nakasima A, Akamine A (2004) Dentin regeneration by dental pulp stem cell therapy with recombinant human bone morphogenetic protein 2. J Dent Res 83:590–595. https://doi.org/10.1177/154405910408300802
Guo W, He Y, Zhang X, Lu W, Wang C, Yu H, Liu Y, Li Y, Zhou Y, Zhou J, Zhang M (2009) The use of dentin matrix scaffold and dental follicle cells for dentin regeneration. Biomaterials 30:6708–6723. https://doi.org/10.1016/j.biomaterials.2009.08.034
Jiao L, Xie L, Yang B, Yu M, Jiang Z, Feng L, Guo W, Tian W (2014) Cryopreserved dentin matrix as a scaffold material for dentin-pulp tissue regeneration. Biomaterials 35:4929–4939. https://doi.org/10.1016/j.biomaterials.2014.03.016
Koga T, Minamizato T, Kawai Y, Miura K, Takashi I, Nakatani Y, Sumita Y, Asahina I (2016) Bone regeneration using dentin matrix depends on the degree of demineralization and particle size. PLoS One 11:e0147235. https://doi.org/10.1371/journal.pone.0147235
Gao X, Qin W, Wang P, Wang L, Weir MD, Reynolds MA, Zhao L, Lin Z, Xu HH (2019) Nano-structured demineralized human dentin matrix to enhance bone and dental repair and regeneration. Appl Sci 9:1013. https://doi.org/10.3390/app9051013
Togari K, Miyazawa K, Yagihashi K, Tabuchi M, Maeda H, Kawai T, Goto S (2011) Bone regeneration by demineralized dentin matrix in skull defects of rats. J Hard Tissue Biol 21:25–34. https://doi.org/10.2485/jhtb.21.25
Smith JG, Smith AJ, Shelton RM, Cooper PR (2012) Antibacterial activity of dentine and pulp extracellular matrix extracts. Int Endod J 45:749–755. https://doi.org/10.1111/j.1365-2591.2012.02031.x
Kim YK, Bang K, Murata M, Mitsugi M, Um IW (2017) Retrospective clinical study of allogenic demineralized dentin matrix for alveolar bone repair. J Hard Tissue Biol 26:95–102. https://doi.org/10.2485/jhtb.26.95
Chen G, Chen J, Yang B, Li L, Luo X, Zhang X, Feng L, Jiang Z, Yu M, Guo W, Tian W (2015) Combination of aligned PLGA/Gelatin electrospun sheets, native dental pulp extracellular matrix and treated dentin matrix as substrates for tooth root regeneration. Biomaterials 52:56–70. https://doi.org/10.1016/j.biomaterials.2015.02.011
Yang B, Chen G, Li J, Zou Q, Xie D, Chen Y, Wang H, Zheng X, Long J, Tang W, Guo W (2012) Tooth root regeneration using dental follicle cell sheets in combination with a dentin matrix - based scaffold. Biomaterials 33:2449–2461. https://doi.org/10.1016/j.biomaterials.2011.11.074
Mirmalek-Sani SH, Sullivan DC, Zimmerman C, Shupe TD, Petersen BE (2013) Immunogenicity of decellularized porcine liver for bioengineered hepatic tissue. Am J Pathol 183:558–565. https://doi.org/10.1016/j.ajpath.2013.05.002
Moharamzadeh K, Freeman C, Blackwood K (2008) Processed bovine dentine as a bone substitute. Br J Oral Maxillofac Surg 46:110–113. https://doi.org/10.1016/j.bjoms.2007.07.209
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed were conducted strictly in full accordance with the ethical principles and standards of the institutional and national research committee and with the 1964 World Medical Association Declaration of Helsinki and its later amendments (version 2008). All experimental protocols were independently reviewed and approved by the Institutional Ethical Committee, Faculty of Dentistry, Alexandria University (IRB No. 00010556-IORG 0008839). This study was registered by the Pan African Clinical Trial Registry (PACTR) managed by Cochrane SA with identification number PACTR201901866476410.
Informed consent
Informed written consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Clinical relevance
This is the first histological study using the treated dentin matrix as a pulp-capping agent on humans showing a positive trend to dentin regeneration.
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Holiel, A., Mahmoud, E., Abdel-Fattah, W. et al. Histological evaluation of the regenerative potential of a novel treated dentin matrix hydrogel in direct pulp capping. Clin Oral Invest 25, 2101–2112 (2021). https://doi.org/10.1007/s00784-020-03521-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-020-03521-z