Abstract
Coronary microvascular remodeling and ischemia in hypertension
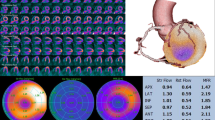
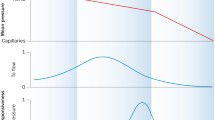
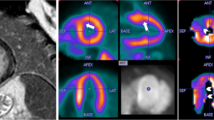
An increasing amount of evidence suggests that the development of myocardial ischemia in hypertensive patients without angiographically demonstrable coronary artery disease, may at least in part be due to anatomic and functional abnormalities of the coronary microvasculature. Studies employing cardiac imaging techniques, in particular positron emission tomography (PET), have demonstrated that the coronary flow reserve (CFR), i.e. the ratio of myocardial blood flow (MBF) during near maximal vasodilatation (pharmacologically-induced) to resting MBF, is significantly impaired in hypertensive patients with or without left ventricular hypertrophy (LVH). In the absence of significant coronary stenoses, an abnormal CFR is suggestive of dysfunction of the coronary microcirculation. In parallel, mechanistic studies have suggested that microvascular dysfunction can be a result of several interacting mechanisms, including myocyte remodeling, vascular (intramyocardial coronary arteriole) remodeling, and decreased vasodilatory capacity of the coronary microcirculatory endothelium.
Furthermore, PET studies of patients with hypertrophic cardiomyopathy have demonstrated that the severity of CFR impairment is an independent predictor of clinical deterioration and death in these patients and may precede clinical deterioration by years. Similarly, preliminary studies in hypertensive patients with or without LVH have suggested that long-term therapy with the combination of the ACE inhibitor, perindopril 2 mg, and the diuretic, indapamide 0.625 mg, may improve the status of coronary microcirculation in these patients, although these findings need to be substantiated in larger studies.
Résumé
Il existe de plus en plus de données qui suggèrent que, chez les patients hypertendus exempts de maladie coronaire objectivée par angiographie, la survenue d’une ischémie myocardique pourrait être liée, au moins en partie, à des anomalies anatomiques et fonctionnelles de la microcirculation coronaire. Des études ayant fait appel aux techniques d’imagerie cardiaque, notamment à la tomographie par émission de positons (PET), ont démontré que la réserve coronaire (RC), c’est-à-dire le rapport du débit sanguin myocardique (DSM) lors d’une vasodilatation sous-maximale (induite pharmacologiquement) sur le DSM de repos, est altérée de manie`re significative chez les patients hypertendus, que ces derniers présentent ou non une hypertrophie ventriculaire gauche (HVG). En l’absence de sténose coronaire significative, une RC anormale témoigne d’une dysfonction de la microcirculation coronaire. Paralle`lement, des études mécanistes semblent indiquer que cette dysfonction microvasculaire pourrait résulter de plusieurs mécanismes intriqués, à savoir le remodelage myocytaire, le remodelage vasculaire (au niveau des artérioles coronaires intramyocardiques) et la diminution de la capacité de vasodilatation de l’endothélium des microvaisseaux coronaires.
De plus, des études par PET menées chez des patients atteints de cardiomyopathies hypertrophiques ont démontre que la sévérité de l’altération de la RC est un facteur prédictif indépendant d’aggravation clinique et de décès chez ces patients et peut précéder la dégradation clinique de plusieurs années. De même, des études préliminaires chez des patients hypertendus présentant ou non une HVG semblent indiquer que, chez de tels sujets, le traitement à long terme par l’association de perindopril (2 mg), un inhibiteur de l’enzyme de conversion (IEC), et d;indapamide (0,625 mg), un diurétique, peut améliorer la microcirculation coronaire, bien que ces données demandent à être confirmées par de plus vastes études.





Similar content being viewed by others
Références
Ringvist I, Fisher LD, Mock M, et al. Prognostic value of angiographic indices of coronary artery disease from the Coronary Artery Surgery Study (CASS). J Clin Invest 1983; 71: 1854–66
Uren NG, Melin JA, De Bruyne B, et al. Relation between myocardial blood flow and the severity of coronary artery stenosis. New Engl J Med 1994; 330: 1782–8
Maseri A. Coronary vasoconstriction: visible and invisible. N Engl J Med 1991; 325: 1579–80
Maseri A, Crea F, Cianflone D. Myocardial ischemia caused by distal coronary vasoconstriction. Am J Cardiol 1992; 70: 1602–5
Pupita G, Maseri A, Kaski JC, et al. Myocardial ischemia caused by distal coronary constriction in stable angina pectoris. N Engl J Med 1990; 323: 514–20
Chilian WM, Eastham CL, Layne SM, et al. Small vessel phenomena in the coronary microcirculation: Phasic intramyocardial perfusion and micro-vascular dynamics. Prog Cardiovasc Dis 1988; 31: 17–38
Marcus ML, Chilian WM, Kanatsuka H, et al. Understanding the coronary circulation through studies at the microvascular level. Circulation 1990; 82: 1–7
Chilian WM, Eastham CL, Marcus ML. Microvascular distribution of coronary vascular resistance in beating left ventricle. Am J Physiol 1986; 251:H779–88
Chilian WM, Layne SM, Eastham CL, et al. Heterogeneous microvascular coronary alpha-adrenergic vasoconstriction. Circ Res 1989; 64: 376–88
Toyota E, Koshida R, Hattan N, et al. Regulation of the coronary vasomotor tone: What we know and where we need to go. J Nucl Cardiol 2001; 8: 599–605
L’Abbate A, Marzilli M, Ballestra AM, et al. Opposite transmural gradients of coronary resistance and extravascular pressure in the working dog’s heart. Cardiovasc Res 1980; 14: 21–9
Sambuceti G, Marzilli M, Fedele S, et al. Paradoxical increase in microvascular resistance during tachycardia downstream from a severe stenosis in patients with coronary artery disease: reversal by angioplasty. Circulation 2001; 103:2352–60
De Silva R, Camici PG. The role of positron emission tomography in the investigation of coronary circulatory function in man. Cardiovasc Res 1994; 28: 1595–612
Camici PG. Positron emission tomography and myocardial imaging. Heart 2000; 83: 475–80
Dutka DP, Camici PG. The contribution of positron emission tomography to the study of ischemic heart failure. Prog Cardiovasc Dis 2001; 43: 399–418
Camici PG, Rimoldi OE. Myocardial blood flow in patients with hibernating myocardium. Cardiovasc Res 2003; 57: 302–11
Schafers KP, Spinks TJ, Camici PG, et al. Absolute quantification of myocardial blood flow with H2 15O and 3-dimentional PET: an experimental validation. J Nucl Med 2002; 43: 1031–40
Kaufmann PA, Gnecchi-Ruscone T, Yap JT, et al. Assessment of the reproducibility and hyperemic myocardial blood flow measurements with 15O_labelled water and PET. J Nucl Med 1999; 40: 1848–56
Kaufmann PA, Gnecchi-Ruscone T, di Terlizzi M, et al. Coronary heart disease in smokers: Vitamin C restores coronary microcirculatory function. Circulation 2000; 102: 1233–8
Brush JE, Cannon RO, Schenke WH, et al. Angina due to coronary microvascular disease in hypertensive patients without left ventricular hypertrophy. N Engl J Med 1988; 319: 1302–7
Schwartzkopff B, Motz W, Frenzel H, et al. Hypertension: Structural and functional alterations of the intramyocardial coronary arterioles in patients with arterial hypertension. Circulation 1993; 88: 993–1003
Galderisi M, de Simone G, Cicala S, et al. Coronary flow reserve in hypertensive patients with appropriate and inappropriate left ventricular mass. J Hypertens 2003; 21: 2183–8
Kozàkovè M, de Simone G, Morizzo C, et al. Coronary vasodilator capacity and hypertension-induced increase in left ventricular mass. Hypertension 2003; 41: 224–9
Treasure CB, Klein JL, Vita JA, et al. Coronary circulation: Hypertension and left ventricular hypertrophy are associated with impaired endotheliummediated relaxation in human coronary resistance vessels. Circulation 1993; 87: 86–93
Chilian WM, Koshida R. EDHF and NO: Different pathways for production -similar actions. Circ Res 2001; 89: 648–9
Matsunaga T, Warltier DC, Weilhrauch DW, et al. Ischemia-induced coronary collateral growth is dependent on vascular endothelial growth factor and nitric oxide. Circulation 2000; 102: 3098–103
Choudhury L, Rosen SD, Patel D, et al. Coronary vasodilator reserve in primary and secondary left ventricular hypertrophy: a study with positron emission tomography. Eur Heart J 1998; 18: 108–16
Cecchi, F, Olivotto I, Gistri R, et al. Coronary microvascular dysfunction and prognosis in hypertrophic cardiomyopathy. N Engl J Med 2003; 349: 1027–35
Mourad J-J, Hanon O, Deverre R-J, et al. Improvement of impaired coronary vasodilator reserve in hypertensive patients by low-dose ACE inhibitor/diuretic therapy: a pilot PET study. J Renin Angiotensin Aldosterone Syst 2003; 4: 94–5
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Camici, P.G. Remodelage microvasculaire et ischémie coronaire dans l’hypertension artérielle. Am J Cardiovasc Drugs 4 (Suppl 1), 25–30 (2004). https://doi.org/10.2165/00129784-200404991-00008
Published:
Issue Date:
DOI: https://doi.org/10.2165/00129784-200404991-00008